Memo
Pennsylvania Medicaid Spending and the Affordable Care Act
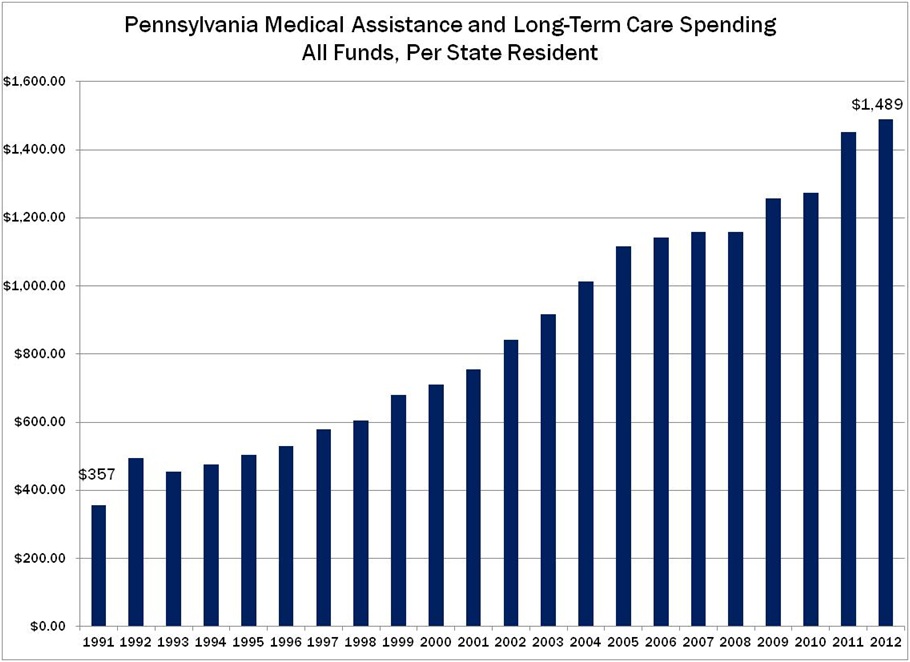
Current Medicaid spending trends are unsustainable. Medicaid spending (Medical Assistance and Long Term Care) consumes about 30 percent of Pennsylvania’s total state operating budget. In the past decade, Medicaid spending increased 83 percent compared to a 45.4 percent increase in Pennsylvanians’ personal income.
Medicaid spending has also outpaced state tax revenue, and costs are projected to continue to grow faster than the economy. Nationally, Medicaid costs will grow by an estimated 6.6 percent until 2020 without the Affordable Care Act, or 8.1 percent if the act is implemented. The Independent Fiscal Office estimates state welfare spending (largely Medical Assistance) will increase by 8 percent per year for the next three years, five times as fast as General Fund revenue.
Without significant changes, Medicaid spending will require new taxes or continue to crowd out education and other state priorities.
How does the Affordable Care Act affect Medicaid? The Affordable Care Act (ACA) expands Medicaid eligibility and limits state Medicaid reform efforts. The ACA requires states to increase eligibility for Medicaid to 133 percent of the Federal Poverty Level for all families. Currently, states maintain various eligibility limits.
In return for expanding eligibility under the ACA, the federal government would pay the full expansion costs from 2014 to 2016 and at least 90 percent of costs thereafter. However, President Obama’s 2013 proposed budget would reduce the share paid by the federal government.
In June, the Supreme Court ruled the federal government cannot force states to increase Medicaid eligibility, making the expansion optional.
The ACA also includes a “Maintenance of Effort” mandate that prevents states from changing current Medicaid eligibility or covered benefits until 2014.
How would the Medicaid expansion impact Pennsylvania? The expansion will add an additional 800,000 individuals to Medicaid, bringing the state’s Medicaid population to about 3 million or one quarter of Pennsylvanians, according to estimates from the Department of Public Welfare.
These newly eligible Pennsylvanians would cost taxpayers more than $21 billion from 2014 to 2022. While federal tax dollars would cover the majority of this cost, Pennsylvania would be on the hook for an estimated $1.3 to $5.5 billion in state taxpayer costs, according to the Heritage Foundation.
How would the ACA impact Medicaid recipients? Medicaid provides low-quality coverage to recipients. Thanks to low doctor reimbursement rates, patients have a difficult time finding a doctor who accepts Medicaid. As a result, Medicaid patients use ERs about twice as often as the uninsured and privately insured. A recent survey in Health Affairs found one third of Medicaid providers refuse new patients even as states expand their Medicaid enrollment, escalating the Medicaid access problem. Some states, including California, are looking to cut doctor payments even further to address Medicaid funding challenges, exacerbating quality concerns.
How are other states responding to the Medicaid expansion? Six states have formally announced they will opt out of Medicaid expansion: Texas, Louisiana, Florida, South Carolina, Georgia and Mississippi. Several other states are leaning against imposing the expansion.
A number of governors have indicated they are willing to accept Medicaid expansion, but only if the federal government offers more flexibility for states in administrating Medicaid, both for those covered under the expansion and flexibility to restructure the current program.
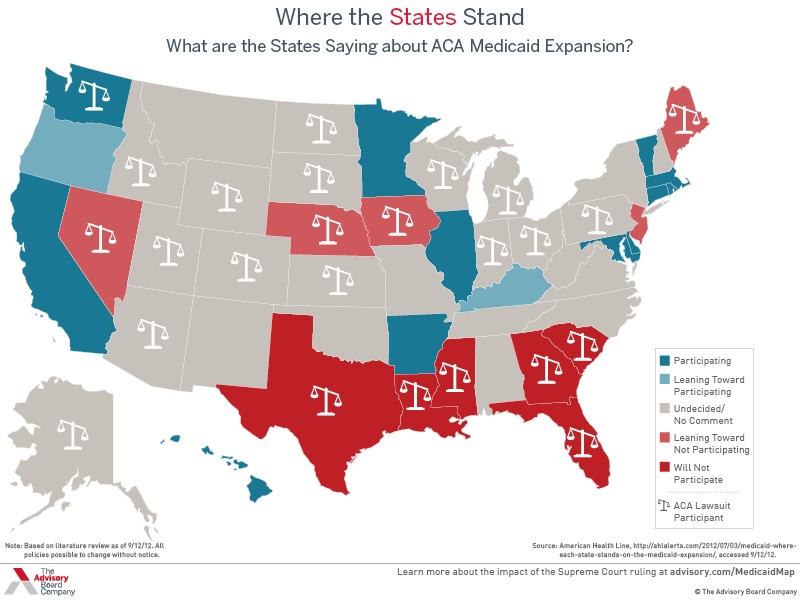
Where does Pennsylvania stand on the Medicaid expansion? Governor Corbett has not taken an official position on the Medicaid expansion. In contrast, 45 members of the Pennsylvania House of Representatives articulated their opposition to expanding Medicaid in a July letter to Governor Corbett. House Majority Whip Stan Saylor has circulated a co-sponsorship memo for legislation that would require Pennsylvania to opt out of the Medicaid expansion under the ACA.
How do we fix Medicaid? Pennsylvania recently took steps to control Medicaid costs, but the only way to bend the cost curve and improve care is regulatory flexibility from the federal government. Without state flexibility to innovate, change incentives and right-size the program, future generations of taxpayers won’t be able to afford a social safety net.
Congress should give Pennsylvania the ability to manage Medicaid through block-grants, or a waiver, allowing state lawmakers to control spending and customize care to meet the unique needs of Pennsylvanians. States like Rhode Island and Florida received federal waivers and were able to restructure Medicaid spending to save money and improve the quality of services.
A proposal like Paul Ryan’s Path to Prosperity would give states their current level of federal Medicaid funds—increased for inflation and population growth—while allowing states the ability to restructure the program to provide better care to recipients at a sustainable cost.
# # #
Elizabeth Stelle is a policy analyst with the Commonwealth Foundation (www.CommonwealthFoundation.org), Pennsylvania’s free-market think tank.